Yes, vision therapy is typically covered by insurance. Vision therapy is a type of treatment that aims to improve specific visual skills such as eye coordination, focusing ability, and visual perception.
It is often recommended for individuals with various vision problems, including lazy eye, crossed eyes, and learning disabilities related to visual processing. As an essential treatment for these conditions, many insurance plans cover vision therapy to some extent. However, the coverage may vary depending on the specific insurance plan and the individual’s diagnosis.
It is recommended to check with your insurance provider to determine the extent of coverage for vision therapy.
Understanding Vision Therapy
Vision therapy is a non-surgical and non-invasive treatment that aims to improve various visual conditions and enhance visual skills. It involves a series of customized exercises and activities, performed under the guidance of a trained eye care professional. Vision therapy is designed to address the root causes of visual problems, rather than simply treating the symptoms. It is a holistic approach that focuses on improving the coordination and efficiency of the visual system.
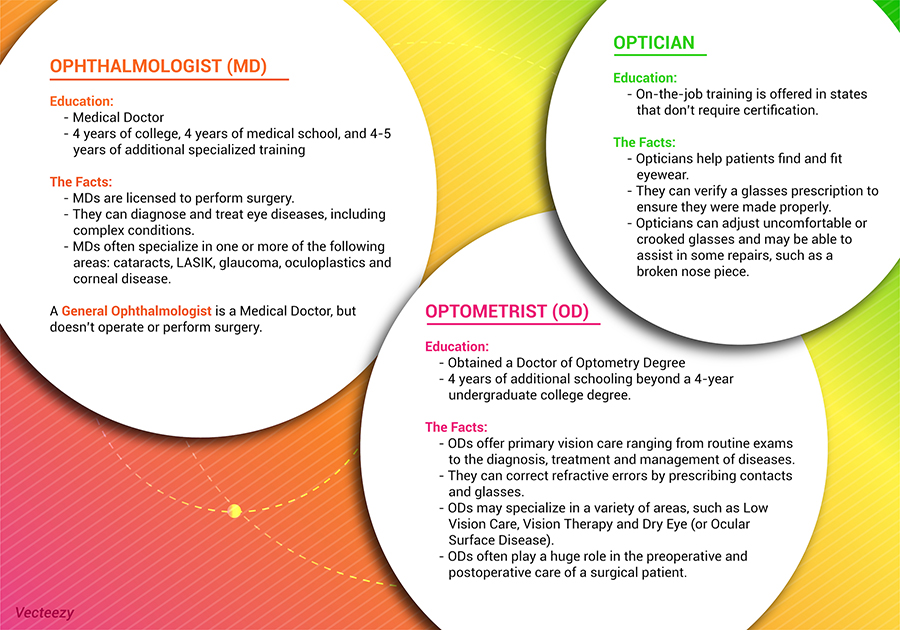
Vision therapy is a structured program that combines a variety of exercises and techniques to address specific visual problems. It is typically prescribed by optometrists or ophthalmologists who specialize in developmental or behavioral optometry. The purpose of vision therapy is to train the eyes and brain to work together more effectively, improving visual skills such as focusing, eye tracking, and depth perception.
Vision therapy can be beneficial for individuals with a wide range of visual conditions, including:
- Strabismus: This is a condition in which the eyes are misaligned or do not work together properly. Vision therapy can help to correct this misalignment and improve eye coordination.
- Amblyopia: Commonly referred to as “lazy eye,” amblyopia occurs when one eye is weaker than the other. Vision therapy can help strengthen the weaker eye and improve visual acuity.
- Binocular Vision Disorders: These are conditions in which the eyes have difficulty working together as a team. Vision therapy can help improve binocular vision, allowing for better depth perception and visual integration.
- Focusing Problems: Vision therapy can assist individuals who struggle with maintaining clear vision at different distances or experience eye strain or headaches during near tasks.
- Eye Tracking Problems: Poor eye tracking skills can contribute to difficulties in reading and comprehension. Vision therapy can help improve eye movement control and tracking abilities.
In summary, vision therapy is a specialized treatment that aims to improve visual skills and address specific visual problems. It targets conditions such as strabismus, amblyopia, binocular vision disorders, focusing problems, and eye tracking issues. By undertaking a tailored program of exercises and activities, individuals can enhance their visual abilities and ultimately enjoy improved quality of life.
Insurance Coverage For Vision Therapy
Vision therapy is a specialized treatment that helps improve visual abilities. Whether or not insurance covers vision therapy depends on the individual policy and provider. It’s important to check with your insurance company to understand the coverage options for vision therapy.
Overview Of Insurance Coverage
One of the primary concerns for individuals seeking vision therapy is whether it is covered by insurance. Insurance coverage can significantly impact the accessibility and affordability of healthcare treatments. In the case of vision therapy, insurance coverage varies depending on a range of factors such as the insurance provider, policy type, and specific eligibility criteria. Understanding the fundamentals of insurance coverage for vision therapy is crucial for individuals seeking this type of treatment.
Factors Affecting Coverage
Several factors influence the extent to which insurance covers vision therapy. It is essential to be aware of these factors to determine the likelihood of obtaining coverage from your insurance provider. Some of the key factors affecting insurance coverage for vision therapy include:
- Type of Insurance Policy: Different insurance policies have varying coverage guidelines. Some policies may explicitly exclude vision therapy, whereas others may provide partial or full coverage.
- Insurance Provider: Each insurance provider has its own policies and guidelines regarding vision therapy coverage. It is crucial to review your specific insurance provider’s policy to understand the extent of coverage they offer.
- Diagnosis and Medical Necessity: Insurance coverage for vision therapy often requires a diagnosis of a specific visual condition and a determination of medical necessity. This means that the treatment must be deemed essential for improving or maintaining visual function.
- Referral and Authorization: Some insurance plans may require a referral from a primary care physician or optometrist before covering vision therapy. Additionally, pre-authorization may be necessary to ensure coverage.
- Out-of-Pocket Expenses: Even if vision therapy is covered by insurance, there may still be out-of-pocket expenses such as copayments or deductibles that need to be considered.
It is essential to thoroughly research and understand your insurance policy’s coverage details regarding vision therapy. This can help you plan and budget accordingly and avoid any potential surprises or unexpected expenses.
Health Insurance Plans And Vision Therapy
Health insurance plans play a crucial role in covering various medical treatments and therapies. However, when it comes to vision therapy, the coverage may vary depending on the type of insurance you have. In this section, we will explore how both private health insurance and government health insurance policies cover vision therapy and highlight any limitations or preauthorization requirements.
Private Health Insurance
Private health insurance plans offered by companies or purchased individually often provide coverage for vision therapy. These plans typically include vision care benefits, which may cover a portion or the entire cost of vision therapy sessions. However, it is essential to review the details of your specific insurance policy to determine the extent of coverage provided.
Private health insurance providers usually have lists of healthcare providers and therapists within their network. It is advisable to consult the insurance company’s website or contact their customer service to confirm if your vision therapist is within the network. Choosing an in-network provider can lead to lower out-of-pocket expenses.
Furthermore, private health insurance plans may require preauthorization for vision therapy services. This means that you must obtain approval from your insurance company before starting the therapy to ensure coverage. It is crucial to familiarize yourself with the preauthorization process and requirements to avoid any unexpected expenses.
Government Health Insurance
Government health insurance programs, such as Medicare and Medicaid, also offer coverage for vision therapy services. However, the coverage and eligibility criteria may differ from private health insurance plans. Medicare typically covers vision therapy if it is deemed medically necessary and prescribed by a qualified healthcare professional.
Medicaid coverage for vision therapy varies between states. Some states provide comprehensive coverage, while others may have restrictions or limitations. It is essential to check your specific state’s Medicaid program guidelines or consult with your healthcare provider to determine the extent of coverage.
Limitations And Preauthorization
Despite health insurance plans offering coverage for vision therapy, there may be limitations on the number of sessions or the duration of coverage. Some insurance plans may have a maximum limit per year or impose restrictions on the age of the individual receiving therapy.
Preauthorization requirements, as mentioned earlier, ensure that the therapy is medically necessary and meets specific criteria set by the insurance provider. It is crucial to reach out to your insurance company, gather the necessary information, and complete the preauthorization process before commencing vision therapy.
Remember, understanding your insurance policy’s coverage for vision therapy can help you make informed decisions about your treatment options and manage your healthcare expenses effectively. Stay proactive by contacting your insurance provider, reading your policy documents thoroughly, and seeking guidance from healthcare professionals.
Credit: www.mneye.com
Vision Insurance Plans And Vision Therapy
In this section, we will discuss the coverage aspects of vision insurance plans and how they relate to vision therapy. Understanding the coverage nuances can help you navigate the insurance landscape and make informed decisions about your vision care.
Coverage Aspects
When it comes to vision therapy, coverage by insurance plans may vary. Some plans may cover vision therapy, while others may have limited or no coverage. The actual coverage details depend on the specific vision insurance plan you have.
It’s important to note that not all insurance plans include vision coverage. In many cases, vision coverage needs to be purchased separately as a stand-alone vision plan. Therefore, if you are considering vision therapy and want insurance coverage for it, make sure you have a vision insurance plan in place or check your existing plan for vision therapy coverage.
Stand-alone Vision Plans
If your employer does not offer vision insurance, or if you’re self-employed or a freelancer, you might need to explore stand-alone vision insurance plans. These plans focus solely on vision care and can be purchased independently or in addition to your existing health insurance plan.
Stand-alone vision insurance plans typically provide coverage for various services and treatments related to vision care, including routine eye exams, prescription eyewear, and even vision therapy. However, it’s crucial to carefully review the plan’s terms and conditions to ensure vision therapy is covered and to understand any limitations or requirements that may apply.
When considering a stand-alone vision plan, take note of the following:
- Check if the plan explicitly mentions coverage for vision therapy.
- Confirm whether the plan has any restrictions or requirements, such as the need for a referral from an eye care specialist.
- Determine if the plan covers the full cost of vision therapy or if there are any out-of-pocket expenses.
- Find out if there are any specific network providers or clinics that the plan requires you to visit for vision therapy services.
By understanding the coverage aspects of stand-alone vision plans, you can ensure that you have the necessary insurance coverage for vision therapy.
Alternative Options For Coverage
When considering vision therapy, many people wonder if insurance will cover this treatment. While coverage may vary depending on your specific insurance plan, there are some alternative options for coverage that you can explore. These options can help alleviate the financial burden and make vision therapy more accessible to you. Two popular alternatives include Flexible Spending Accounts (FSAs) and Health Savings Accounts (HSAs).
Flexible Spending Accounts (fsas)
If you have a Flexible Spending Account (FSA) through your employer, you may be able to use these funds to cover the cost of vision therapy. FSAs allow you to set aside pre-tax dollars from your paycheck to pay for qualified medical expenses, which can include vision therapy. By using the funds in your FSA, you can save money on taxes and reduce your out-of-pocket expenses for vision therapy.
Health Savings Accounts (hsas)
Another alternative option for coverage is Health Savings Accounts (HSAs). HSAs are available to individuals who have a high-deductible health insurance plan. These accounts allow you to contribute pre-tax dollars into a savings account, which can be used to pay for qualified medical expenses, such as vision therapy. Like FSAs, HSAs offer a tax advantage and enable you to save money while receiving the necessary treatment.
Before utilizing an FSA or HSA for vision therapy, it is important to check with your plan provider to ensure that this type of treatment is eligible. Some insurance plans may require a prescription or documentation from a licensed healthcare professional to qualify for reimbursement. Therefore, it is crucial to consult with your healthcare provider and insurance company to understand the specific requirements and guidelines for using these alternative options for coverage.
Overall, Flexible Spending Accounts (FSAs) and Health Savings Accounts (HSAs) offer viable alternatives for covering the cost of vision therapy. These options can help make the treatment more affordable and accessible, allowing individuals to receive the necessary care without straining their finances. By taking advantage of these alternative options, you can prioritize your vision health and invest in the therapy you need.

Credit: www.facebook.com
Out-of-pocket Expenses For Vision Therapy
When it comes to vision therapy, one of the most common concerns is the cost and whether it is covered by insurance. While many insurance plans do cover vision therapy to some extent, there are often out-of-pocket expenses involved. In this article, we will delve into the cost of vision therapy sessions and explore budgeting and financing options for those considering this treatment.
Cost Of Vision Therapy Sessions
Understanding the cost of vision therapy sessions is crucial before embarking on this treatment. Every practice may have different fee structures, and the total cost can vary depending on various factors such as location, duration of treatment, and complexity of the condition being treated. On average, a vision therapy session can range from $75 to $150 per session.
It’s important to note that vision therapy is usually not a one-time affair. It typically involves multiple sessions over a period of several weeks or months. The number of sessions required will depend on the specific needs of the individual and the progress made throughout the treatment.
Budgeting And Financing Options
Considering the potential out-of-pocket expenses, it’s essential to explore budgeting and financing options for vision therapy. To make this treatment more affordable, here are a few strategies:
- 1. Check Insurance Coverage: Start by checking your insurance coverage and finding out what benefits are offered for vision therapy. Contact your insurance provider and ask if they cover vision therapy and what percentage of the cost they will reimburse. Remember to ask about any specific requirements or documentation needed for reimbursement.
- 2. Flexible Spending Accounts (FSAs) or Health Savings Accounts (HSAs): These accounts allow you to set aside pre-tax money to cover medical expenses. Check if vision therapy is considered an eligible expense under your FSA or HSA. If so, you can use these funds to pay for the treatment, potentially reducing your out-of-pocket expenses.
- 3. Payment Plans: Talk to your vision therapist about the possibility of setting up a payment plan. Many practices offer flexible payment options that allow you to spread out the cost of treatment over a period of time. This can alleviate the burden of paying a large sum upfront.
- 4. Healthcare Financing: If you need assistance in financing vision therapy, you may consider healthcare financing options. These specialized financing programs are designed to help individuals cover medical expenses that may not be fully covered by insurance. Research different healthcare financing companies to find one that suits your needs.
By exploring these budgeting and financing options, you can make vision therapy more affordable and accessible. Remember, investing in your vision health can have long-term benefits, so it’s important to explore all resources available to you.
Credit: www.ecurtisdesigns.com
Frequently Asked Questions On Is Vision Therapy Covered By Insurance
How Is Vision Therapy Billed?
Vision therapy is billed through insurance providers or on a fee-for-service basis.
Why Does Vision Therapy Cost So Much?
Vision therapy can be costly due to several factors such as specialized equipment, highly trained therapists, personalized treatment plans, and the duration of the therapy. It is a specialized service that requires expertise and resources, resulting in its higher cost compared to other treatments.
Is Vision Therapy Medically Necessary?
Yes, vision therapy can be medically necessary for certain conditions. It is a non-surgical treatment that helps improve visual skills and coordination. Consult with an eye care professional to determine if vision therapy is suitable for your specific needs.
What Conditions Are Treated By Vision Therapy?
Vision therapy is used to treat conditions such as lazy eye, crossed eyes, reading and learning difficulties, and binocular vision problems.
Conclusion
The coverage of vision therapy by insurance providers can vary depending on the specific plan and company. It is imperative for individuals to thoroughly review their insurance policies or contact their providers to determine if vision therapy is covered. By conducting proper research and taking the necessary steps, patients can navigate their insurance coverage and ensure they have access to the vision therapy they need for optimal eye health.



