Yes, spinal decompression may be covered by insurance.
Credit: www.prophysiomt.com
Types Of Spinal Decompression
Spinal decompression can be of different types, including traction, surgical decompression, and non-surgical decompression. When it comes to insurance coverage, it is important to check with your provider as coverage may vary.
Types of Spinal Decompression When it comes to treating chronic back pain, spinal decompression has gained popularity as an effective method. But before considering this treatment, it’s important to understand the different types of spinal decompression techniques available. In this article, we will explore the two main types of spinal decompression: nonsurgical and surgical, and discuss their differences, benefits, and insurance coverage.Nonsurgical Spinal Decompression
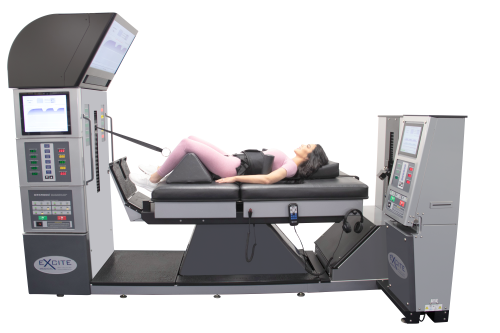
Nonsurgical spinal decompression is a non-invasive approach that aims to relieve pressure on the spinal discs and nerves. This technique is often recommended for individuals suffering from conditions such as herniated discs, degenerative disc disease, sciatica, and spinal stenosis. During the nonsurgical spinal decompression procedure, the patient lies on a special table that is designed to gently stretch and decompress the spine. This gentle traction helps to create negative pressure within the affected disc, promoting the retraction of bulging or herniated material while facilitating the influx of essential nutrients and oxygen. Although nonsurgical spinal decompression is considered a safe and effective treatment option, it may require multiple sessions to achieve optimal results. The number of sessions needed can vary based on the severity of the condition and the individual’s response to treatment.Surgical Spinal Decompression
In some cases, nonsurgical spinal decompression may not provide sufficient relief or the condition may be too severe to be effectively treated without surgery. In such instances, surgical spinal decompression may be recommended. Surgical spinal decompression involves removing a portion of the affected disc, bone, or tissue that is placing pressure on the spinal cord or nerves. This procedure aims to create more space for the compressed structures, relieving pain and improving overall function. It’s important to note that surgical spinal decompression is typically considered a last resort when conservative treatments have failed to provide adequate relief. This is because surgery carries inherent risks and a longer recovery period compared to nonsurgical approaches.Insurance Coverage For Spinal Decompression
When it comes to insurance coverage for spinal decompression, it’s essential to check with your specific insurance provider and policy. Insurance coverage eligibility can vary based on the type of spinal decompression procedure, the underlying condition being treated, and individual insurance policies. While nonsurgical spinal decompression may be covered by certain insurance plans, surgical spinal decompression is more likely to be covered under medically necessary circumstances. In both cases, it’s important to consult with your healthcare provider and insurance company beforehand to determine what is covered and what expenses you may be responsible for. In conclusion, understanding the different types of spinal decompression techniques is crucial in exploring your treatment options for chronic back pain. Whether you opt for nonsurgical or surgical spinal decompression, it’s essential to have a clear understanding of your insurance coverage beforehand to avoid any unexpected financial burdens. Remember to consult with your healthcare provider and insurance company to determine the most appropriate treatment approach and ensure coverage eligibility.
Credit: elevatewellnessdc.com
Requirements For Insurance Coverage
When considering spinal decompression treatment, one common concern that patients have is whether or not it is covered by their insurance. Insurance coverage for spinal decompression can vary depending on several factors, including the patient’s insurance plan and the specific criteria set by the insurance provider. Understanding the requirements for insurance coverage can help patients navigate the process successfully and potentially save on treatment costs.
Meeting Medical Necessity Criteria
Insurance providers generally require treatments to meet certain medical necessity criteria to be eligible for coverage. In the case of spinal decompression, this means that the treatment must be deemed medically necessary for the patient’s specific condition. Medical necessity is typically determined by several factors, including the severity of the condition, the failed attempts at other conservative treatments, and the potential benefits that spinal decompression can offer in terms of pain relief and functional improvement.
Patients should consult their insurance policy or contact their insurance provider directly to find out the specific medical necessity criteria they need to meet for coverage. The insurance company may ask for documentation from the healthcare provider supporting the medical necessity of spinal decompression, such as medical records, diagnostic imaging results, and a detailed treatment plan.
Obtaining Prior Authorization
Prior authorization is another important requirement for insurance coverage of spinal decompression. It is the process in which the healthcare provider and the insurance company discuss and obtain approval for the proposed treatment before it is carried out. Without prior authorization, the insurance company may deny coverage for the procedure or may limit the coverage amount.
To obtain prior authorization, the healthcare provider usually needs to submit a request to the insurance company, along with the necessary documentation supporting the medical necessity of spinal decompression. The insurance company will review the request and make a determination based on their coverage policies. It is essential for patients to initiate this process well in advance to ensure smooth approvals and prevent any delays in treatment.
It is important to note that not all insurance plans cover spinal decompression, and even if the treatment is covered, there may be limitations, such as a specific number of sessions or a requirement for a trial period of conservative treatments before considering spinal decompression. Patients should thoroughly review their insurance policies or consult with their insurance providers to understand the specific coverage details and any financial responsibilities they may have.
By understanding and fulfilling the requirements for insurance coverage, patients can increase the chances of receiving financial assistance for spinal decompression treatment. Consulting with the healthcare provider and insurance company early in the process can help navigate the paperwork and ensure a smoother experience.
Credit: www.swankchiro.com
Frequently Asked Questions For Is Spinal Decompression Covered By Insurance
Why Is Decompression Not Covered By Insurance?
Decompression is not covered by insurance because it is considered an elective procedure.
How Much Does A Spinal Decompression Cost?
The cost of spinal decompression varies but typically ranges from $1,000 to $5,000 per session. Prices may differ based on factors like location, provider, and additional treatments required. It’s best to consult with a healthcare professional to determine the exact cost for your specific condition and treatment plan.
What Is The Success Rate Of Spinal Decompression?
Spinal decompression has a success rate of around 60-80%. It helps relieve pain by gently stretching the spine, creating negative pressure that allows discs to retract. This therapy can be effective for conditions like herniated discs, sciatica, and degenerative disc disease.
How Do You Bill For Spinal Decompression?
Spinal decompression is usually billed through insurance or directly by the healthcare provider. Insurance companies may cover the cost if it is deemed medically necessary. The provider will typically submit a claim with the necessary codes for reimbursement.
Conclusion
Determining if spinal decompression is covered by insurance can be a complex process. It is important to thoroughly review your insurance policy and consult with your provider to understand the specific coverage available. While some insurance plans may provide coverage for spinal decompression, others may consider it an elective procedure.
Ultimately, exploring your options and seeking clarification from your insurance provider is crucial to making informed decisions about your healthcare.




